Hospitals throughout our region are reporting a surge of COVID-19 cases over the last few weeks.
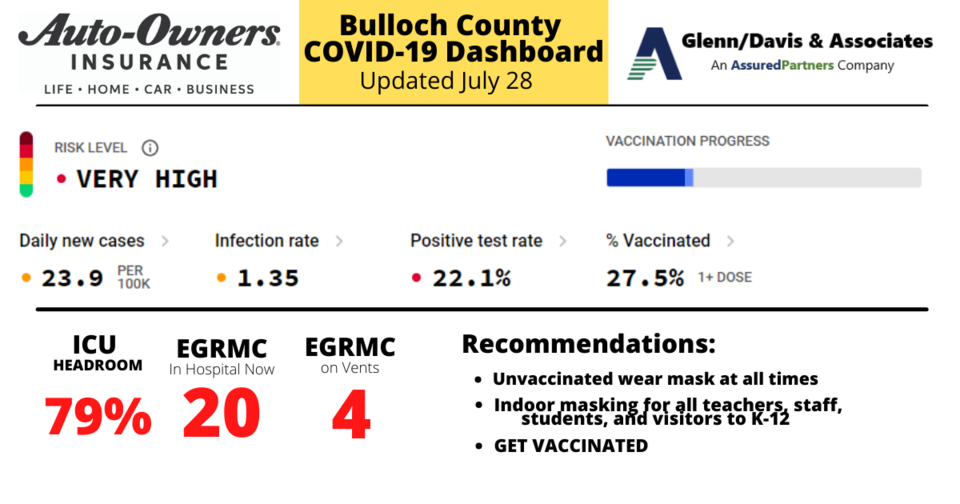
East Georgia Regional Medical Center reported 20 COVID-19 patients Wednesday - 4 of which are on vents. Bulloch EMS is reporting high call volume of potential COVID patients. Many area hospitals have been in and out of diversion due to the new influx of COVID patients on top of other patients.
Since Monday, COVID-19 cases in Bulloch County have increased by 62.
One local urgent care reported seeing 113 patients yesterday. 85 of the 113 were tested for COVID. Urgent cares and other providers are experiencing a shortage of testing supplies and are struggling to keep enough supplies in to meet the demand. Some of them may start limiting the number of daily test because of this surge of COVID-19.
DPH is doing free PCR COVID testing three days a week. Ted Wynn, Director of Bulloch County Public Safety has received no notification from DPH of plans to increase local testing to help meet the surge in demand.
Providers are reporting increasing interest in Vaccines. That is the best way to defeat this virus and stop this surge.
Until then, the CDC has issued revised mask guidance recommending that even vaccinated people should wear masks indoors in communities of high spread of COVID infection. Bulloch spread level is currently listed as VERY HIGH.
The CDC is now recommended that everyone age two and up should wear mask when returning to school.
COVID Hospitalizations (MAJORITY ARE UNVACCINATED):
- East Georgia Medical Center - 20
- Memorial Medical Center - 44
- St. Joseph's - 18
- Candler Hospital (SAV) - 20
Region J which extends from Augusta to Brunswick is reporting surge of COVID-19:
- Region J has 215 ICU beds in use out of a total of 231 total ICU beds, or 93.07%.
- Region J has 284 ED beds in use out of 329 total beds, or 86.32%
- Region J has 942 general inpatient beds in use out of 1,086 total beds, or 86.74%
GET VACCINATED NOW
Safer Activities for You and Your Family
- If you are fully vaccinated, you can participate in many of the activities that you did before the pandemic.
- To maximize protection from the Delta variant and prevent possibly spreading it to others, wear a mask indoors in public if you are in an area of substantial or high transmission. (Bulloch is VERY HIGH now)
- Wearing a mask is most important if you have a weakened immune system or if, because of your age or an underlying medical condition, you are at increased risk for severe disease, or if someone in your household has a weakened immune system, is at increased risk for severe disease, or is unvaccinated. If this applies to you or your household, you might choose to wear a mask regardless of the level of transmission in your area.
- You should continue to wear a mask where required by laws, rules, regulations, or local guidance.
CDC Key Takeaways for Schools
Given new evidence on the B.1.617.2 (Delta) variant, CDC has updated the guidance for fully vaccinated people. CDC recommends universal indoor masking for all teachers, staff, students, and visitors to K-12 schools, regardless of vaccination status. Children should return to full-time in-person learning in the fall with layered prevention strategies in place.
- Students benefit from in-person learning, and safely returning to in-person instruction in the fall 2021 is a priority.
- Vaccination is currently the leading public health prevention strategy to end the COVID-19 pandemic. Promoting vaccination can help schools safely return to in-person learning as well as extracurricular activities and sports.
- Masks should be worn indoors by all individuals (age 2 and older). Consistent and correct mask use by people is especially important indoors and in crowded settings, when physical distancing cannot be maintained.
- CDC recommends schools maintain at least 3 feet of physical distance between students within classrooms, combined with indoor mask wearing by people who are not fully vaccinated, to reduce transmission risk. When it is not possible to maintain a physical distance of at least 3 feet, such as when schools cannot fully re-open while maintaining these distances, it is especially important to layer multiple other prevention strategies, such as indoor masking.
- Screening testing, ventilation, handwashing and respiratory etiquette, staying home when sick and getting tested, contact tracing in combination with quarantine and isolation, and cleaning and disinfection are also important layers of prevention to keep schools safe.
- Students, teachers, and staff should stay home when they have signs of any infectious illness and be referred to their healthcare provider for testing and care.
- Many schools serve children under the age of 12 who are not eligible for vaccination at this time. Therefore, this guidance emphasizes implementing layered prevention strategies (e.g., using multiple prevention strategies together consistently) to protect people who are not fully vaccinated, including students, teachers, staff, and other members of their households.
- COVID-19 prevention strategies remain critical to protect people, including students, teachers, and staff, who are not fully vaccinated, especially in areas of moderate-to-high community transmission levels.
- Localities should monitor community transmission, vaccination coverage, screening testing, and occurrence of outbreaks to guide decisions on the level of layered prevention strategies (e.g., physical distancing, screening testing).